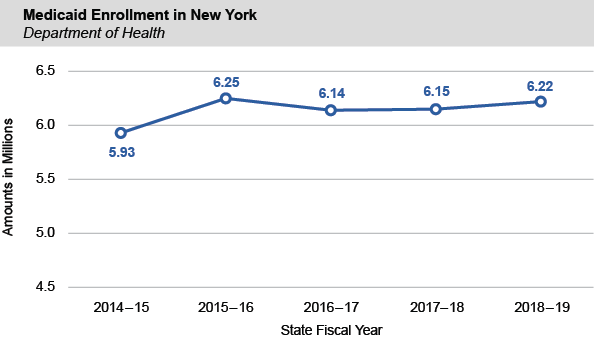
Department of Health Medicaid Enrollment Ticks Up by One Percent
- Average monthly Department of Health (DOH) Medicaid enrollment exceeded 6.2 million in SFY 2018-19, an increase of 62,825 recipients, or 1.0 percent, compared to the prior year. The increase reflects higher enrollment among all eligibility groups, except the blind and disabled.
- Compared to the prior year, average monthly DOH Medicaid enrollment for:
- Adults increased by 18,449 (0.8 percent) to nearly 2.5 million;
- Children with Medicaid coverage increased by 4,470 (0.2 percent) to nearly 2.2 million;
- Elderly recipients increased by 19,875 (3.2 percent) to 642,769;
- Blind or disabled recipients decreased by 1,269 (0.2 percent) to 686,902; and
- Other eligible recipients—primarily persons who were not born in the U.S. and who are not naturalized citizens—increased by 21,300 (11.6 percent) to 204,246.
- Average monthly DOH Medicaid managed care enrollment in SFY 2018-19 increased by 39,776 (0.8 percent) to over 4.7 million, or 76.3 percent of all recipients, compared to the year before. This increase largely reflects steady growth in managed long-term care enrollment and the continued transition of eligible recipients to Health and Recovery Plans (HARPs) for adults with mental health or substance use disorders, offset in part by a decrease in mainstream Medicaid managed care enrollment.
Medicaid Spending Increases, Largely Due to Additional Federal Payments from the Federal Affordable Care Act (ACA)
- Compared to the year before, combined local, State and federal Medicaid spending increased by $3.1 billion (4.4 percent) to $72.5 billion in SFY 2018-19. This increase largely reflects additional federal Medicaid payments, most of which are associated with the ACA. The decline in State share spending is influenced by a deferral of certain Medicaid payments with a State-share total of $1.7 billion from March 2019 to April 2019, which according to the Division of the Budget was necessary to ensure compliance with the global cap limit for SFY 2018-19.
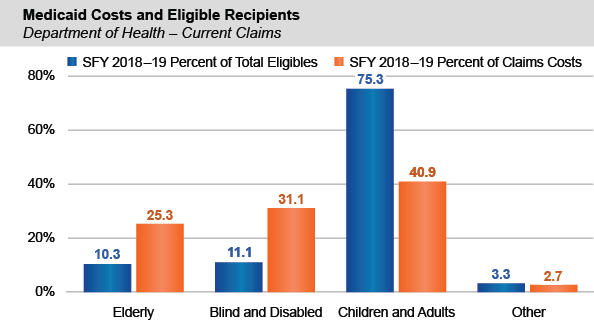
- Children and adults represented 75.3 percent of all average monthly DOH Medicaid enrollees, but only 40.9 percent of the costs of DOH Medicaid claims for the State in SFY 2018-19. Elderly, blind and disabled enrollees made up 21.4 percent of eligible recipients, but accounted for 56.4 percent of DOH Medicaid claims costs.
The Essential Plan Continues to Grow
- In SFY 2018-19, enrollment in the Essential Plan averaged 773,584,* an increase of 44,777 (6.1 percent) over the prior year.
- In 2015, New York State joined Minnesota to become the only states in the nation to establish a Basic Health Program, a new low-cost health insurance option authorized by the ACA and largely funded by the federal government. In New York State, the Basic Health Program is known as the Essential Plan.
- The Essential Plan is available to individuals who are under 65, not eligible for Medicaid or the Child Health Plus (CHP) Program, without access to affordable coverage and with incomes at or below 200 percent of poverty.
- In SFY 2018-19, federal funds covered 98.1 percent or nearly $4.1 billion in Essential Plan costs, with State funds covering the remaining 1.9 percent. Individuals with incomes greater than 150 percent but at or below 200 percent of poverty pay $20 monthly premiums to private health plans participating in the program. Individuals with incomes at or below 150 percent of poverty have no monthly premium.
- All participating health plans cover inpatient and outpatient care, physician services, diagnostic services and prescription drugs with low out-of-pocket costs and no annual deductible. Enrollees have no out-of-pocket costs for preventive care, including routine office visits and recommended screenings.
Over 7.4 Million New Yorkers Benefit from DOH Medicaid, Essential Plan or CHP
- In January 2019, over 7.4 million individuals or more than one in three New Yorkers were enrolled in DOH Medicaid, the Essential Plan or CHP.
* Reflects preliminary unaudited results.